The process of a growing a human inside you can cause many weird and wonderful things to happen to your body. Increased weight, a change in your posture and some pretty significant hormonal changes can mean that a few twinges here and there are to be expected. One area of pain that is very common in pregnancy is pelvic girdle pain (PGP); usually felt as a pain in the butt or groin. But being common doesn’t make it normal, nor does it make it untreatable. So what is PGP and what can you do about it?
What is Pelvic Girdle Pain?
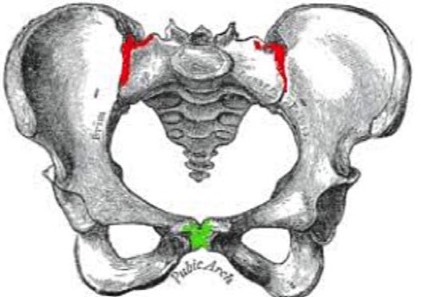
Pelvic girdle pain refers to pain that originates from one or more of the joints in the pelvis. There are three main joints – 2 sacroiliac joints at the back and 1 pubic symphysis joint at the front. All of these joints are capable of giving you pain. The sacroiliac joints can give pain at the back of the pelvis and the pubic symphysis can produce pain at the front/deep in the groin.
What causes it?
Pelvic girdle pain is often caused by dysfunction in the pelvic joints. This is more common during pregnancy, with up to 76% of all pregnant women suffering from some form of pelvic girdle pain. The pain is more common in pregnancy because: – Hormones released in pregnancy cause the ligaments to relax and the pelvic joints to move more in preparation for childbirth – Increased movement of the joints and a weakening of the ‘core stability’ muscles can reduce the body’s ability to keep these joints stable = A change in the body’s centre of gravity, posture and weight can place additional strain on these joints
What does it feel like?
Symptoms of pelvic girdle pain often start around 18 weeks of pregnancy and usually peak between 24 and 36 weeks.
Sacroiliac joint pain
Usually feels like: – Deep and sometimes ‘stabbing’ pain in the buttock/back of the pelvis – Usually one-sided pain, although the side can change
Pubic symphysis pain
Usually feels like: -Deep groin pain that can almost feel ‘internal’ and can also radiate down the inner thigh
What aggravates it?
Most types of pelvic girdle pain are aggravated by:
- Standing
- Walking
- Climbing stairs
- Resting weight on one leg
- Getting in and out of a low chair or the car
- Lying flat on your back
- Rolling in bed
- Lifting
How can you treat it?
To manage your pain, it is important that you first have the pain properly assessed and diagnosed. Once diagnosed, your physio will discuss your specific management. Treatment might include:
- massage
- manual therapy
- exercises, including strengthening and stretching
- postural education
- advice on activity modification
- bracing / taping
Additional tips to manage the pain
- Avoid standing with your weight on one leg
- Wear supportive shoes
- Avoid asymmetrical positions, like crossing your legs
- Do regular pelvic floor exercises
- Use functional bracing by tightening your pelvic floor and deep abdominal muscles before moving
Lying down
- Avoid lying on your back for long periods, especially on a hard surface like the ground
- When lying on your side, try placing a pillow between your knees and another under your tummy
Turning over in bed
- Bend your knees up, brace your pelvic floor and deep abdominal muscles and roll with your knees and hips together
Getting out of the chair
- Make sure both feet are on the ground evenly
- Sit on the edge of your seat Brace your pelvic floor and deep abdominal muscles, lean your weight forward and push up with your arms if possible
Getting out of the car
- Swing your legs out of the car first so that both feet are on the ground before standing up
GLOW specialises in treating pre and postnatal pain, including pelvic girdle pain. We use a range of techniques, including hands on treatment, exercise and bracing with pelvic support belts to have you feeling better asap!
Recommended reading from Glow
How long does it take to get my body back after having a baby?
3 reasons you should practise breathing
5 habits for a happy, healthy spine!
5 simple exercises to kick-start your day!
